25 Jan What If You Don’t Like Your Midwife?
What do you do if you don’t like your midwife? It’s not always an easy road.
I recall being a little disappointed at how clinically she read out the questions from the paperwork. The question, “When was the date of your last period?” was read in exactly the same tone and with the same lack of eye contact as “Have you ever suffered from depression or suicidal thoughts?”
I only just made it into the birth-centre program in my local public hospital – or so the lady on the phone told me. I was only five weeks’ pregnant, but apparently if I’d waited another week to phone, I would have gone on the waiting list.
So that’s how I came to be granted a much sought after spot on the birth-centre program. I felt pretty lucky and relieved that I was ‘in’. The information pack explained that the program was free, apart from the cost of one ultrasound. We read that when the time came, we would get our own “homely” room in which to give birth. Afterwards, we could snuggle as a family in the double bed without being interrupted. I would be allocated a midwife who would support me through the entire pregnancy, the labour and the two weeks following the birth. She would come to my house for appointments at times that suited me.
The leaflet explained that forming a relationship with one midwife has been shown to increase the likelihood of a positive birth outcome for both mother and baby. It made sense to me.
Contrast this to the public maternity ward upstairs from the birthing centre where I knew there were long waits for routine antenatal appointments, no guarantee of your own room following the birth, and nowhere for dads to sleep, and it was easy to see why the birthing centre program was favoured by most women.
It was my first pregnancy, and my husband and I were pretty chuffed. When I was 13 weeks’ pregnant, I met my midwife – let’s call her Jackie. She came to our house one evening to start the ball rolling with some forms and questions. My husband had arranged some bickies on a plate and offered her a cuppa, both of which she declined.
I recall being a little disappointed at how clinically she read out the questions from the paperwork. The question, “When was the date of your last period?” was read in exactly the same tone and with the same lack of eye contact as “Have you ever suffered from depression or suicidal thoughts?” I noticed a long pause and a slightly confused look on her face whenever we asked anything.
I guess I had had visions of a warm, nurturing type who would be excited about the pregnancy with us. It wouldn’t be fair to describe her as rude, or even cold. There was just no… connection.
The pregnancy continued uneventfully. Jackie took measurements; she ordered the glucose test and ultrasound. There was still no real bonding happening between us, but I felt she knew her stuff as a midwife and I told myself that that was the most important thing. It really wasn’t her job to nurture me; it was her job to help me have a healthy baby.
Around week 24 of my pregnancy, I came out in a torturous red rash that covered my entire body.
The rash was so itchy that after the first night with it, I wanted to be knocked out until it went away. I discovered that itchiness is almost impossible to ignore unless, perhaps, you happen to be a meditation master, which I certainly was not. Being pregnant, unfortunately there weren’t many medical options available to me to relieve the torture, and the cold oatmeal baths recommended by the pharmacist just didn’t cut it.
I checked the list that Jackie had given us detailing when we were allowed to call her on her mobile and when we had to wait until our next appointment. I decided this was serious enough to call. Not only was I going mad with the rash, I was really worried about the baby. I was also pretty tired and teary by this stage, and although some reassurance and sympathy would have been nice, it seemed I was not going to get it from Jackie.
I wanted her to say, ‘You poor thing’ or ‘I’ve seen this before – don’t worry, it’s nothing’ or even ‘You need to go to the hospital immediately’.
I wanted her to take control of the situation and tell me what to do. Instead, she said, well… nothing much. There was another long pause. She suggested I could go to my GP the next day. She said she didn’t know what it could be. She didn’t once acknowledge that I was struggling just to get words out through my tears on the other end. I hung up feeling like a big cry-baby.
Thankfully, it appeared that nothing serious had caused the rash. It started to improve after three very long weeks, but my ambivalence towards Jackie didn’t.
At one appointment with Jackie, I wanted to talk about the different pain-relief options we had learned about in the prenatal class the week before. I mentioned that I didn’t really have a ‘birth plan’ because I wanted to keep my options open and not rule anything out. I said that I hoped I wouldn’t need an epidural but that if I wanted one I would ask for it. After all, this was my first baby and I had no idea how painful it would be (but I had an inkling it was going to hurt a lot).
Although my husband says she wasn’t quite this harsh, what I heard her say at the end of this conversation about pain relief was, “Well, if you’re already thinking about an epidural, you’re probably not right for this program”. Suddenly I was wondering the same thing myself.
I was also starting to wonder, during my appointments with Jackie and during the prenatal classes, whether there was a reluctance among some (not all) of the birthing-centre midwives to seek help from a doctor unless absolutely necessary.
It was as though having to use intervention that required a doctor (such as an epidural) reflected in some way a failing of the program or of their skills.
I understood the challenges midwives have faced in being recognised as highly competent, and I agreed with their position that the less intervention in childbirth the better. I was more than happy to be assisted solely by a midwife and my husband during my labour. I just wanted to know that they would call for a doctor if I wanted one, without hesitating because of how this would reflect on them or the program.
By this stage, I was 36 weeks’ pregnant. I considered asking for a different midwife at the birth centre as we had been told at the start it was perfectly fine to do so.
Call me unassertive, but I just couldn’t face the awkwardness of bumping into Jackie after switching midwives in such a small program. Plus, I was beginning to get nervous about the pain and wanted to know I could have an epidural if I wanted one.
Without adequate private-health-insurance cover, my only other option was to have the baby ‘upstairs’. Already, one of the couples in our prenatal group had been sent ‘upstairs’ due to some issues with the pregnancy and we all felt a bit sorry for them. Still, I secretly made an appointment there for the next day (secretly, because I wasn’t ready to give up my spot on the program).
I’m pretty sure I was the first person ever to consider voluntarily giving up their place on the birth-centre program, since they asked me several times if I had been asked to make the appointment by Jackie because of complications with my pregnancy.
They seemed perplexed when I said nothing was wrong medically, I had just changed my mind about where I wanted to have my baby.
I can’t explain why, but after that first appointment ‘upstairs’, I knew I wanted to have my baby there. Every midwife I had contact with was fantastic. Still, it was really hard to give up my spot. It was as though I was turning down a great job that I had beaten more than a hundred applicants for. Even harder was phoning Jackie to tell her.
I told Jackie that I just wanted to have all the options available to me in terms of pain relief as it was my first baby and I didn’t know what to expect. She was uncharacteristically kind, which almost made me think I’d made a terrible misjudgement.
Maybe she had felt the lack of connection between us too, and was happy I was leaving.
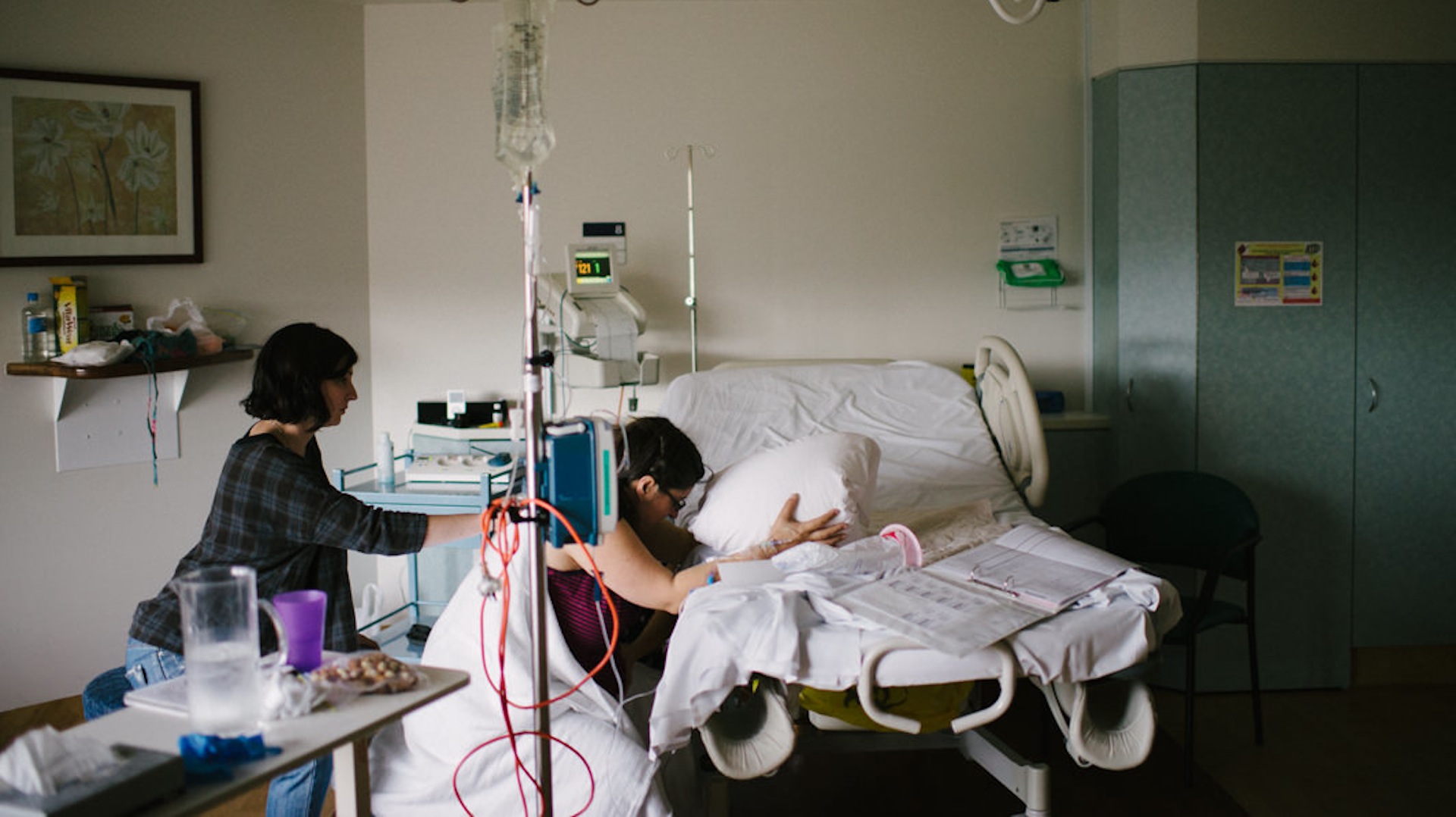
At 11.30 pm one Valentine’s Day, I finally (at 42 weeks) went into labour. By the time I arrived at the hospital two hours later, I was in another place (I think it’s called the World of Pain). A midwife with thick red glasses helped me to a birthing suite. It didn’t have a double bed with nice music playing, but I couldn’t have cared less about my surroundings at that point. “I want an epidural,” I managed to grunt.
First she gave me a shot of pethidine, which I was thankful for, but which I have to say didn’t do a whole lot. After checking how dilated I was, she leaned over me and whispered, “The bad news is that it’s too late for an epidural, and the good news is that it’s time to have your baby”. I don’t know why, but I trusted her immediately. She gently talked me through the next stage and involved my husband in everything.
It was just the three of us… until after about half an hour when there were four. Just like that.
So as it turned out, I probably would have been absolutely fine in the birth centre with Jackie. After all, it was so quick that an epidural wasn’t possible, and I didn’t need a doctor. Instead, a lady with red glasses whom I had never met ended up as my midwife. Although I’m sure she told me, I didn’t even know her name until later – Marg.
In a weird way, I think it helped that Marg and I had never met. She had no preconceived ideas about me and I had none about her. To be honest, I also felt reassured by the clinical feel of the busy hospital ward with beeping machines and doctors flitting around the place. It wasn’t ideal sharing a small room with another new mum and her baby that first night, but I was so besotted with my baby that it didn’t matter all that much.
I saw Marg with the red glasses once after that, when she popped in to say hello. I thanked her and we took a photo of her with the baby. Then she left. I remember thinking how she had just shared one of the most profound experiences of my life, yet I might never see her again – apart from in our photo album.
I wish there were enough places at every birth centre for every woman who would like to have their child in one.
I wish every woman who wanted her own room with a double bed after giving birth could have one, no matter whether she was in a birth-centre program or not. I wish we could all choose where we give birth and how much pain relief we want, without being judged for our preferences.
For me, instinct told me that giving up my place on the birth-centre program was the right thing to do.
The most important consideration as to where to give birth, I believe, is that you need to feel safe. You need to know you will be listened to. The reality is that it is the luck of the draw when it comes to giving birth – you can have a positive or difficult experience no matter where you have your baby – but as long as you feel safe, you are in the right place.
Words By Kate Triglone




